Crystal formation in the blood is a sclerotic process that is related to inflammation. The presence of crystalline forms is often associated with high blood pressure, plaque and atherosclerosis. There are often WBCs attached and attracted to crystal formations in the blood, attempting to engulf the crystals. This is a favourable sign and an indication of an active immune system.
short_description
Crystal formation in the blood is a sclerotic process that is related to inflammation. The presence of crystalline forms is often associated with high blood pressure, plaque and atherosclerosis. There are often WBCs attached and attracted to crystal formations in the blood, attempting to engulf the crystals. This is a favourable sign and an indication of an active immune system.
appearance
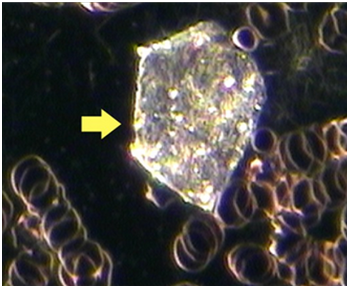
Cholesterol crystals are trapezoidal structures of varying sizes that appear semi-opaque in brightfield and reflective in darkfield. They are typically greyish in colour in brightfield and due to the semi-opaque nature of the crystal RBCs are often visible under a part of the crystal. A typical cholesterol crystal also normally has two adjacent sides that form a sharp, well-defined edge or corners.
associated_symptoms
- May be asymptomatic
- Fatigue
- Poor circulation
- Angina
- Family history of hypercholesterolemia
general_guidelines
- Increase water intake. To determine necessary daily water intake (in litres): Weight (kg) / 8) x 0.25.
- Increase intake of fibre-rich carbohydrates (those tolerated by the blood type) and raw, polyunsaturated fats.
- Avoid saturated fat, refined carbohydrates and food deficient in natural enzymes.
- Avoid alcohol, caffeine, sugar, drugs and non-essential medication.
- Raw vegetable juices, sprouts, greens and antioxidant-rich superfoods.
- Increase essential minerals and electrolyte intake: Bio-lonic Mineral Concentrate (Neogenesis Health Products).
- Test & treat high cholesterol if high.
- Follow a diet appropriate for high cholesterol
- Increase intake of soluble fibre
- Test and correct Homocysteine.
medical_perspective
It is widely accepted that hypercholesterolemia, or more accurately, higher concentrations of LDL and lower concentrations of functional HDL are strongly associated with cardiovascular disease because these promote atheromatous plaque development in arteries. Atherosclerosis leads to myocardial infarction, stroke and peripheral vascular disease. The total serum cholesterol level and LDL:HDL ratio is mostly determined by genetic factors, but weight, medication, food choices, physical activity, etc. also have an impact.
Atheromatous plaques were initially referred to as fatty streaks by pathologists. However, they are not composed of fat cells, but rather of accumulations of white blood cells (especially macrophages) that have taken up oxidized low-density lipoprotein (LDL). After they accumulate large amounts of cytoplasmic membranes (with associated high cholesterol content) they are termed foam cells. When foam cells die, their contents are released, which attracts more macrophages and creates an extracellular lipid core near the centre to inner surface of each atherosclerotic plaque. Conversely, the outer, older portions of the plaque become more calcific, less metabolically active and more physically stiff over time. This process continues, while the plaque increases in size, until it completely occludes an artery.
pleomorphic_perspective
These are Sclerosymplasts (or crystalline symplasts) and form through the process of systatogeny. In the process of systatogeny a number of colloids which can be in different developmental stages, fuse to create a more stable form. The excess colloids are then effectively withdrawn from traffic. Through dehydration they become dry, sclerotic protein forms that are very resistant to extreme temperatures (Enderlein called them terrifying or permanent forms). These are usually associated with hindrances in blood circulation. The colour of the reflective inclusions indicates the system that is burdened:
Green = urogenital tract and kidneys;
Yellow and Brown = upper abdomen, liver, gall bladder
Cornflower Blue = thyroid gland.
implications
- Indication of possible high serum cholesterol.
- Possible excessive saturated fat intake.
- Inadequate lipid metabolism due to lipase deficiency.
- Atherosclerotic plaque.
- Associated Symptoms:
- May be asymptomatic
- Fatigue
- Poor circulation
- Angina
- Family history of hypercholesterolemia
interventions
Any combination of the following, depending on the rest of the case:
LIVER PROTOCOL:
- Avoid alcohol, caffeine, tobacco, saturated/animal fat, sugar, drugs and non-essential medication.
- Hepaton (Neogenesis Health Products): 30 drops tincture 3x daily. May be increased to 5ml tincture 3xdaily.
SUPPLEMENTS:
- Omega-3 supplement (1000-2000 EPA daily)
- Vitamin E: start with 400mg daily and gradually increase to 800mg daily.
- Buffered vitamin C (2500mg).
- Lipotropic factors
- Carnitine
- Co-Enzyme Q10
- Vitamin B3
working_with
Hypercholesterolemia is very prevalent and is believed to be strongly connected to the development of cardiovascular disease.
For this reason it is very closely monitored by conventional medicine. The safe levels for LDL and the LDL:HDL ratio have been adjusted by the WHO for better management of cardiovascular risk. However, cholesterol-lowering statin drugs have many side-effects, including blocking the production of the important cardiovascular antioxidant Co-Enzyme Q10. Recent research has implicated inflammation and raised homocysteine as more sensitive and earlier indicators for cardiovascular disease risk. In blood analysis signs of inflammation, increased blood viscosity, platelet aggregation and thrombosis risk can be easily detected. These factors are very important in a client’s total cardiovascular disease risk profile and may be more important to address than a slightly raised LDL level alone. Most patients with raised cholesterol levels have an underlying liver imbalance and it is nearly impossible in these cases to correct the cholesterol level naturally without addressing the liver issue.
further_investigations
- Liver function test (LFT)
- Lipogram
- Homocysteine
- Circulatory studies may be necessary including plethysmographic and doppler evaluation, electrocardiograph, angiogram and phonocardiography.
 Disclaimer
Disclaimer