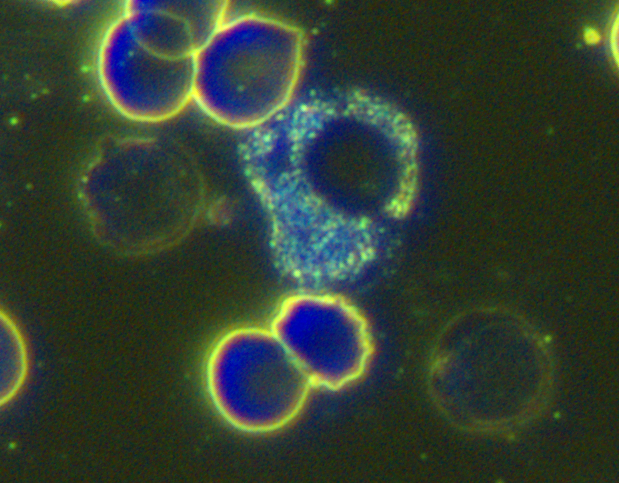

Basophils are the least common circulating white blood cells (<1 % of leukocytes) and the hardest to spot. They’re slightly smaller than neutrophils, packed with large, deep-purple (almost black) granules that often obscure the bilobed nucleus – they look like someone dropped ink blots on the slide.
How they come about
Produced in the bone marrow alongside eosinophils and mast cells, driven by the same IL-3 and IL-5 signals. They’re manufactured in tiny numbers because their tissue cousins (mast cells) do most of the heavy lifting.
What they do
Walking bags of histamine, heparin, and inflammatory mediators. When triggered (usually by IgE antibodies binding allergens), they degranulate explosively and kick off immediate hypersensitivity reactions: itching, swelling, bronchoconstriction, hives, and anaphylaxis in extreme cases. Think of them as the “panic button” of the allergic response.
Where they can go
They spend only a few hours in circulation before migrating into tissues, where they quickly transform into tissue mast cells. Favourite hangouts: skin, lungs, gut lining, and anywhere allergens like to land first.
Lifespan
- In blood: 6–12 hours
- Once in tissues (as mast cells): months to years
In practice
You almost never see basophils in healthy blood. Spotting even one or two per session is abnormal and usually means:
- Acute allergic reaction (food, drug, insect sting)
- Chronic urticaria or severe atopic state
- Parasitic infection (especially if eosinophils are also raised)
- Rarely: certain leukaemias or myeloproliferative disorders
When a basophil shows up under the scope it’s like the blood quietly whispering: “Something is making me really, really itchy on the inside.” Treat it as a loud allergy/parasite alert.
Appearance
Dark purple granules obscuring nucleus
Relevance
Almost never seen in health; any visible = significant
Implications
Severe allergy, parasitic infection (rare)
Interventions
Same as eosinophilia
 Disclaimer
Disclaimer